Amicable1996
Lab Scientist : I'm A Positive And Resourceful Individual Who Can Execute Difficult Tasks And Doesn't Need To Be Micromanaged. Am A Resolute And Dependable Person With Unwavering Determination To Do Well At My Job And Solve Problems In The Most Autonomous Manner Possible. I Am A Passion Driven Personality With Managerial, Entrepreneurial, Leadership, Communication And Interpersonal Skill.
Wants to meet Laboratory Scientist
Articles
14
Followers
4
Connect with me
profile/6213IMG_20211120_124314_487.jpg.webp
Amicable1996
Neanderthals, Environment, And Evolution Behind SARS-CoV-2 Immune Responses
~3.6 mins read
Research led by the Université Paris Cité, CNRS, France, has investigated factors driving variability in diverse immune responses to SARS-CoV-2.
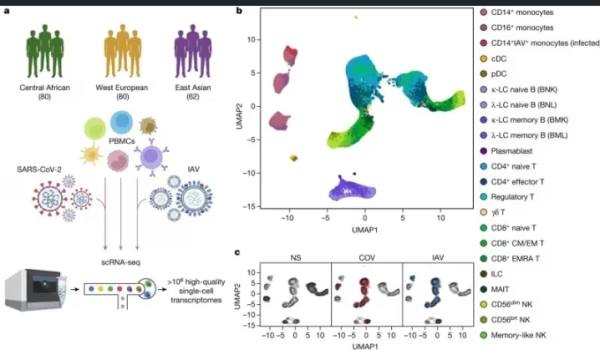
In a paper, "Dissecting human population variation in single-cell responses to SARS-CoV-2," the team used single-cell RNA sequencing to analyze blood cells from diverse populations, comparing responses to SARS-CoV-2 against factors like genetics, age, sex, and comorbidities.
The study investigated immune responses to SARS-CoV-2 and the factors that could contribute to population differences in responses. With 222 healthy blood donors from different geographical regions and ancestries, researchers performed single-cell RNA sequencing on peripheral blood mononuclear cells to analyze their transcriptional responses to SARS-CoV-2 and influenza A virus exposure.
The findings reveal that SARS-CoV-2 induces weaker but more varied interferon-stimulated gene activity than the influenza A virus and has a unique pro-inflammatory signature in myeloid cells.
The findings, published in Nature, also illustrate that variability in population genetics, demographics and environment could explain why susceptibility to SARS-CoV-2 is not uniform.
Age
Older individuals generally exhibited weaker immune responses, which likely contributed to increased susceptibility and severity of COVID-19.
Comorbidities
Individuals with underlying health conditions showed altered immune responses, potentially leading to higher susceptibility and poorer outcomes.
Immune cell type composition
The study points out how proportions of memory cells in lymphoid lineages differ in individuals of African, European, and East Asian descent, potentially contributing to population disparities in cellular activation states.
For instance, African donors presented higher proportions of CD16+ monocytes and memory lymphocyte subsets, such as memory B cells and effector CD4+ T cells.
Environmental exposures
Past viral encounters, such as cytomegalovirus (CMV) infection, were seen to illicit differences in immune responses among different populations.
As an environmental factor, exposure to a virus can be a local or regional occurrence. Without knowledge of these exposures, immune response differences could be correlated to ancestry. The authors warn that this could lead to overestimating the effects of genetic ancestry on immune response variation.
For example, the team found that past CMV exposure accounts for up to 73% of the differences in immune cell proportions between African and European donors. These cell type compositions can impact transcriptional responses to SARS-CoV-2 but are environmental, not genetic in origin.
Genetic factors
Analysis revealed that genetics had a range of response effects on different cell types and immune responses. Common genetic variants can contribute to variations in immune response, but these effects are more pronounced in specific genes that show strong population differentiation.
An example is the rs1142888-G allele, which leads to higher expression of GBP7 in Europeans. This genetic difference likely arose due to positive selection in Europe thousands of years ago that could have been caused by past environmental exposure to pathogens.
Specific genetic variants that are associated with COVID-19 risk, in genes like IRF1, IFNAR2, and DR1, all influence type I interferon signaling, indicating the importance of efficient interferon signaling for favorable clinical outcomes.
Neanderthals
Past comingling and introgression of archaic human genes have contributed to present-day immune responses to SARS-CoV-2. Known Neanderthal genes have been retained in both European and East Asian populations that are specifically related to countering viral threats.
The researchers also identified previously unreported signals of Neanderthal introgression affecting immunity phenotypes. For example, a gene variant that decreases post-translational modification responses to SARS-CoV-2 and IA was found in 38% of Europeans and 22% of East Asians.
Another introgressed variant found in 43% of East Asians and less than 3% of Europeans downregulates a negative regulator of the cytosolic RNA-induced IFN response allowing more interferon release to counter the viral infection.
A Neanderthal haplotype reaching 61% frequency in East Asians and 24% in Europeans, tagged by rs9520848-C allele, is associated with higher basal expression of the cytokine gene TNFSF13B by a subset of T cells.
A Neanderthal genetic variant containing the rs2177336-T allele increases MUC20 expression in SARS-CoV-2-stimulated respiratory cells, particularly for CD4+ T cells. This was linked to decreased COVID-19 susceptibility in Eurasians.
The conserved nature of these archaic introgressions illustrates the deep history of pathogenic viruses testing human immune systems throughout evolution. While science and technology have created distinctly modern strategies to combat viral infections, there may be clues for applying that technology in the evolutionary and introgressively conserved genes.
Insights
The single-cell approach used in the study captured the complexity of immune responses across individuals and populations, revealing the interplay between environmental, genetic, and evolutionary factors.
Importantly the study unentangles the correlations between ancestry and recent environmental influences and illustrates how the environmental factors of the past influence inherited genetics.
With these factors elucidated, we can see how the immune system responds to an immediate novel threat and how it builds and maintains these responses over evolutionary time scales.
profile/6213IMG_20211120_124314_487.jpg.webp
Amicable1996
Fructose And It's Connection With Obesity
~3.3 mins read
Obesity has become a significant health concern worldwide, with a dramatic increase in its prevalence over the past few decades. The complex nature of obesity involves various factors, including genetics, lifestyle, diet, and environmental influences. Among the dietary components that have garnered attention in relation to obesity is fructose, a natural sugar found in fruits, honey, and many processed foods. In this essay, we will explore the connection between fructose consumption and obesity, examining the mechanisms, scientific studies, and potential implications for public health.
Fructose is a monosaccharide, or simple sugar, which is naturally found in fruits, some vegetables, and plant-derived sweeteners like honey and agave. It is also a component of sucrose (table sugar) and high-fructose corn syrup (HFCS), a common sweetener used in many processed foods and beverages. While fructose itself is not inherently harmful, the quantity and context in which it is consumed are essential factors in understanding its potential impact on health.
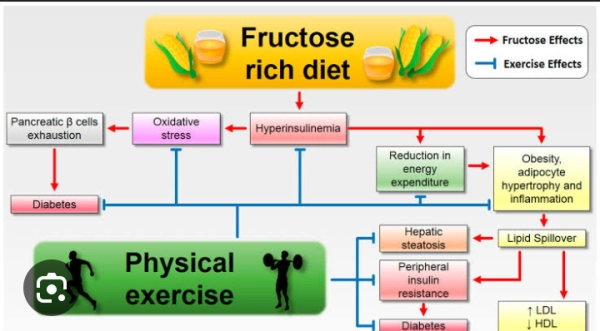
One of the key concerns regarding fructose consumption and obesity is the effect on metabolic processes. Unlike glucose, another simple sugar that is a primary energy source for the body, fructose is metabolized differently. When we consume glucose, it's primarily absorbed by cells throughout the body, including muscle cells, where it can be used for energy or stored as glycogen. However, fructose is primarily metabolized in the liver, where it can contribute to the production of fats (lipogenesis) and increase triglyceride levels, potentially leading to fatty liver disease and insulin resistance.
Several studies have investigated the relationship between fructose consumption and obesity. Some of these studies suggest that excessive fructose intake may contribute to weight gain, especially when consumed in the form of sugary beverages. High consumption of fructose-sweetened beverages has been linked to an increased risk of obesity, type 2 diabetes, and other metabolic disorders. It's essential to note that these studies often focus on the excessive consumption of added sugars, including fructose, rather than the natural sugars found in whole fruits.
A 2019 review published in the journal "Advances in Nutrition" discussed the impact of fructose on obesity. The review highlighted that excessive fructose intake, especially in the form of added sugars, can lead to an increase in overall caloric intake, reduced satiety (feeling of fullness), and a higher likelihood of developing insulin resistance. These factors, when combined, can contribute to weight gain and obesity.
The concept of "sugar addiction" has also been proposed in the context of fructose consumption. Some researchers suggest that excessive sugar intake, including fructose, can activate reward centers in the brain, leading to a cycle of craving and overconsumption, which may contribute to obesity. However, the idea of sugar addiction is still a topic of debate within the scientific community, and more research is needed to fully understand its implications.
It's important to emphasize that not all sources of fructose are equal in their impact on health. Whole fruits, despite containing fructose, provide essential nutrients, dietary fiber, and antioxidants. The fiber in fruits slows down the absorption of sugars, leading to a more gradual rise in blood sugar levels and promoting satiety. Additionally, the vitamins and minerals found in fruits are essential for overall health.
The concern arises when fructose is consumed in excessive amounts from processed foods, sugary beverages, and foods high in added sugars. These sources of fructose often lack the beneficial components present in whole fruits, leading to a more rapid spike in blood sugar levels and potentially contributing to overconsumption.
Public health initiatives have recognized the need to address excessive sugar consumption to combat obesity. Some countries have implemented policies to reduce the consumption of sugary beverages by imposing taxes on sugary drinks or implementing restrictions on marketing unhealthy foods to children. These measures aim to reduce the overall consumption of added sugars, including fructose, which could have a positive impact on obesity rates.
In conclusion, the connection between fructose consumption and obesity is a complex topic that requires careful consideration of various factors. While fructose itself is a natural sugar found in fruits and honey, excessive consumption of added sugars, including fructose in the form of high-fructose corn syrup, has been associated with an increased risk of obesity and metabolic disorders. It's essential to differentiate between the sugars naturally present in whole fruits and the added sugars in processed foods. Public health efforts to reduce the consumption of sugary beverages and promote a balanced diet can play a crucial role in addressing the obesity epidemic. As our understanding of the relationship between fructose and obesity continues to evolve, further research will be essential to guide effective strategies for preventing and managing this global health issue.
Advertisement

Link socials
Matches
Loading...
